Summary
Intrathecally applied fluorescein is used to achieve intraoperative visualization of CSF leaks. This protocol describes a lumbar puncture, the application of 5% fluorescein, and intraoperative visualization using a fully digital microscope.
Abstract
In cases of cerebrospinal fluid (CSF) leaks, reliable detection of their origins is needed to seal the leak sufficiently and prevent complications, such as meningitis. A method is presented here using intrathecal administered fluorescein in a clinical case of bilateral congenital ear malformation. A fluorescent dye is administered intrathecally to achieve intraoperative visualization of CSF leaks. The dye is applied 20 min before surgery, and concentration of 5% is used. Per every 10 kg of body weight, 0.1 mL of the fluid is applied intrathecally. The fluorescein is visualized using a fully digital microscope. The origin of the fluid leak is identified in the stapes footplate. During primary surgery, it is sealed, and cochlea implantation is performed for hearing restoration. In this specific case, 6 weeks later, the implant was explanted due to acute meningitis, and the electrode array was left as a spacer. Postoperatively, in the aural smear, β-transferrin was detected. During a revision mastoidectomy, dislocated coverage of the leak was found. The stapes was removed and oval window sealed. Five days after revision surgery, no β-transferrin was detected in the aural smear. During the revision of cochlea implantation 6 months later, intact coverage of the oval niche was observed. Thus, intrathecal fluorescein application proves to be a reliable tool for the detection of CSF leaks. It facilitates the orientation in malformations and complicated or unknown surgical situs. In the literature, its use is described for CSF fistulas in endonasal surgery but is rarely described in skull base and mastoid surgeries. The method has been used successfully in several cases with CSF leaks, and the results confirm the feasibility of safely accessing the origin of the leak.
Introduction
CSF leaks can be caused by trauma, preexist congenitally, or appear spontaneously. Clinically, they appear via otoliquorrhea or rhinoliquorrhea and can be confirmed by positive β-transferrin secretion1,2. In cases of CSF leaks, reliable detection of its origin is needed to seal the leak sufficiently and prevent complications, such as meningitis.
Intrathecal fluorescein application (IFA) has been known to be highly sensitive in detecting CSF leaks after neurosurgical skull base operations3. However, there is no common consensus on its exact applications (e.g., concentration, amount of fluid, addition of other drugs such as dexamethasone)3,4. A majority of cases describe transnasal endoscopic skull base surgery, while a standardized method of visualizing CSF leaks in the temporal bone via microscopy5,6,7 is missing. These leaks frequently occur at multiple localizations and bear the risk of recurrence if their whole extent is not visualized during surgery8. Specifically, a transmastoid approach only has been found to bear the risk of recurrent leaks8.
This protocol presents the use of intrathecal administered fluorescein via a transmastoid approach. A clinical case of bilateral congenital ear malformation (right ear: cochlear aplasia, left ear: incomplete partition type I), in which minor trauma led to perforation of the left stapes footplate in the middle ear, is also presented. A similar case has only been reported once9.
Subscription Required. Please recommend JoVE to your librarian.
Protocol
This protocol was approved by the local ethics committee in accordance with the Helsinki Declaration (Reg. No. A2019-0214). Informed consent was obtained from all participants. In the presented case involving a child, written informed consent was obtained from both parents.
NOTE: Fluorescein is a fluorescent dye that emits green light (520-530 nm) when stimulated with blue light (of wavelength ~485 nm). It is used for visualization of the tear film in ophthalmology. Its intrathecal use is off-label and based on an individual therapeutic agreement. Fluorescein-Natrium at a 10% concentration is available and regularly used in fluorescein angiography of the ocular fundus in ophthalmology.
1. Preparation for surgery
- Obtain audiological testing, high resolution computed tomography (HRCT), and magnetic resonance imaging (MRI) of the skull base.
- Obtain written, informed consent from the patient regarding off-label use of fluorescein.
- Perform a lumbar puncture and place a lumbar drain for later application of the dye.
- Use fluorescein sodium (10% concentration). For lumbar application, dilute the fluorescein to 5% concentration with water.
- Apply 0.1 mL of the dilution per 10 kg of body weight, with a maximum of 1 mL, intrathecally.
- Perform the application immediately before surgery to achieve intraoperative visualization.
NOTE: When applying the method to children, the application should be performed under general anesthesia. - Perform general anesthesia according to the patient's individual clinical history and risk factors and according to the decision of the anesthesiologist.
- Cover the microscope with a blue light filter to visualize the fluorescein, or use a fully digital microscope.
- Use sterile draping to cover the patient.
2. Surgery
- For the transmastoid approach, perform a mastoidectomy and posterior tympanotomy.
- Expand the surgery according to the expected origin of the leak.
- As a first landmark, expose the dura to the middle cranial fossa.
- Thin the posterior canal wall of the outer ear canal.
- Expose the short incus process in the antrum and identify the lateral semicircular canal.
- Expose the chorda facial angle at which the chorda tympani leaves the facial nerve.
- Open the facial recess. Leave the facial nerve with a bony coverage.
- Access the middle ear through a posterior tympanotomy. The origin of the fluid leak can easily be identified in the stapes footplate (Figure 2).
- Use fascia from the temporal muscle and absorbable collagen fibrin sealant patches to seal the CSF leak until no more fluid leaves the footplate. The stapes suprastructure stabilizes the sealant.
Subscription Required. Please recommend JoVE to your librarian.
Representative Results
In the presented case, minor trauma led to a CSF leak from the nose in a 10 month-old child. Magnetic resonance imaging (MRI) revealed a bilateral temporal bone malformation with aplasia of the right cochlea and dilation of the left cochlea and vestibule with absent interscalar septum identical to an incomplete partition type one. Accordingly, brainstem-evoked audiometry was performed (Figure 1) and confirmed bilateral deafness.
Since high resolution computed tomography (HRCT) did not reveal the origin of the CSF leak, fluorescein-assisted transmastoidal otobasal exploration with simultaneous cochlear implantation was indicated. During primary surgery, the transmastoidal approach was used to identify the CSF in the stapes footplate (Figure 2) to seal the leak and perform cochlea implantation to restore hearing.
Six months after surgery, the child suffered from meningitis caused by mastoiditis. The implant was removed, and the electrode array was left as a spacer. Postoperatively, the aural smear detected β-transferrin10. Revision mastoidectomy was performed showing dislocated coverage of the leak in the stapes footplate. The stapes was completely removed (Figure 3), and the oval window was sealed using temporal muscle, temporal fascia, and absorbable collagen fibrin sealant patches. The stapes was investigated under an electron microscope, showing the malformed footplate with perforations. To reduce pressure on the leak, a lumbar puncture was performed daily. Five days after revision, no β-transferrin was detected. During cochlea implant revision 6 months later, coverage of the oval niche was intact.
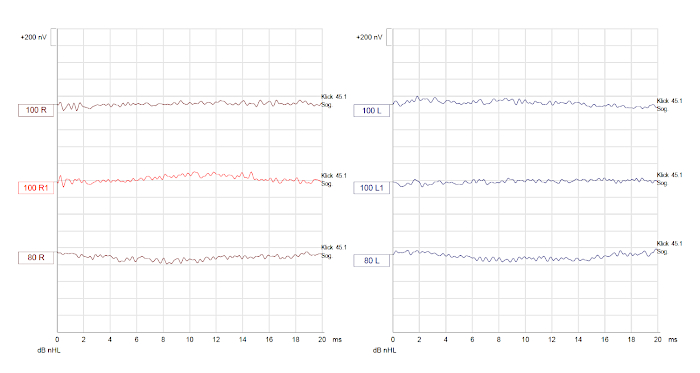
Figure 1: Audiometric results. Brainstem-evoked response audiometry (BERA) showing no reproducible brainstem responses, confirming bilateral deafness. Please click here to view a larger version of this figure.

Figure 2: Identification of the leak in the left stapes footplate. Asterisk: horizontal semicircular canal, arrow: facial nerve. Please click here to view a larger version of this figure.

Figure 3: Extraction of the stapes. Asterisk: lateral semicircular canal, arrow: stapes footplate, cross: eminentia pyramidalis. Please click here to view a larger version of this figure.

Figure 4: Electron microscope investigation of the extracted stapes. Shown is the electron microscopic investigation of the extracted stapes with the congenital perforation. Scale bar indicates the magnification. Please click here to view a larger version of this figure.
Subscription Required. Please recommend JoVE to your librarian.
Discussion
While many reports concerning CSF leaks focus on transnasal endoscopic approaches in skull base surgery, a standardized method of visualizing CSF leaks of the temporal bone via microscopy5,6,7 is lacking. This protocol describes an adaption of existing literature reviews for use in microscopic ear surgery.
The application of fluorescein has been described as a safe method in skull base surgery and uses endoscopic techniques. Side effects are assumed to depend on the dose11. Though the use is off-label, no side effects were observed in all patients receiving intrathecal fluorescein. Furthermore, the dye can be applied repeatedly. No severe long-term side effects are typically expected12. In the literature, intrathecal use of fluorescein is described for CSF fistulas in endonasal surgery13 but is rarely described in skull base and mastoid surgery. Especially in transmastoid surgery, CSF leaks may occur in a multilocular manner and tend to recur8. Waiving a visualization method may lead to recurrent leaks or insufficient sealing methods.
Intrathecal fluorescein is used for cases in which CSF leaks have been confirmed but cannot be visualized via CT or MRI13. Its intrathecal use is proved to be a reliable tool for the detection of CSF leaks11,12,14. It facilitates the orientation in malformations and complicated or unknown surgical situs. This method has been used successfully in several of cases involving CSF leaks, and the results confirm the feasibility of safely accessing the origin of the leak.
The protocol does not require drastic changes in common surgical methods. The only additional effort that must be performed is the lumbar drain. We consider the advantages in visualization highly superior to the potential disadvantages concerning the small risk of a lumbar puncture.
Subscription Required. Please recommend JoVE to your librarian.
Disclosures
The authors declare no financial disclosures.
Acknowledgments
No funding was received.
Materials
| Name | Company | Catalog Number | Comments |
| Fluorescein ALCON 10% injection solution | NOVARTIS | 1467007 | |
| External lumbar drain catheter Silverline | Spiegelberg | ELD33.010.02 | |
| Otologic instruments (round knifes, hooks, curette, sickle knife, microscissors and microforceps) | Spiggle und Theis | No further specification; instruments can vary between the clinics and their use depends on the surgeon's preferation | |
| Surgical microscope ARRISCOPE 1.0 | ARRI Medicals | NA | |
| Consumables | No further specification; material of the standard equipment of the operating clinic can be used | ||
| Water to rinse | |||
| Antifog solution | |||
| Cotton pads | |||
| Cottonoid pledges | |||
| Gown | |||
| Gloves | |||
| Mask | |||
| Suction tubes | |||
| Blade |
References
- Gacek, R. R., Gacek, M. R., Tart, R. Adult spontaneous cerebrospinal fluid otorrhea: diagnosis and management. The American Journal of Otology. 20 (6), 770-776 (1999).
- Schraven, S. P., Bisdas, S., Wagner, W. Synchronous spontaneous cerebrospinal fluid leaks in the nose and ear. The Journal of Laryngology and Otology. 126 (11), 1186-1188 (2012).
- Raza, S. M., et al. Sensitivity and specificity of intrathecal fluorescein and white light excitation for detecting intraoperative cerebrospinal fluid leak in endoscopic skull base surgery: a prospective study. Journal of Neurosurgery. 124 (3), 621-626 (2016).
- Englhard, A. S., Volgger, V., Leunig, A., Messmer, C. S., Ledderose, G. J. Spontaneous nasal cerebrospinal fluid leaks: management of 24 patients over 11 years. European Archives of Oto-rhino-laryngology. 275 (10), 2487-2494 (2018).
- Sieskiewicz, A., Lyson, T., Rogowski, M., Mariak, Z. Endoscopic management of cerebrospinal fluid rhinorhea. The Polish Otolaryngology. 63 (4), 343-347 (2009).
- Liu, H., et al. The use of topical intranasal fluorescein in endoscopic endonasal repair of cerebrospinal fluid rhinorrhea. Surgical Neurology. 72 (4), 341-345 (2009).
- Javadi, S. A. H., Samimi, H., Naderi, F., Shirani, M. The use of low- dose intrathecal fluorescein in endoscopic repair of cerebrospinal fluid rhinorrhea. Archives of Iranian Medicine. 16 (5), 264-266 (2013).
- Cheng, E., Grande, D., Leonetti, J. Management of spontaneous temporal bone cerebrospinal fluid leak: A 30-year experience. American Journal of Otolaryngology. 40 (1), 97-100 (2019).
- Tandon, S., Singh, S., Sharma, S., Lahiri, A. K. Use of Intrathecal Fluorescein in Recurrent Meningitis after Cochlear Implantation. Iranian Journal of Otorhinolaryngology. 28 (86), 221-226 (2016).
- Warnecke, A., et al. Diagnostic relevance of beta2-transferrin for the detection of cerebrospinal fluid fistulas. Archives of Otolaryngology - Head & Neck Surgery. 130 (10), 1178-1184 (2004).
- Keerl, R., Weber, R. K., Draf, W., Wienke, A., Schaefer, S. D. Use of sodium fluorescein solution for detection of cerebrospinal fluid fistulas: an analysis of 420 administrations and reported complications in Europe and the United States. The Laryngoscope. 114 (2), 266-272 (2004).
- Keerl, R., Weber, R. K., Draf, W., Radziwill, R., Wienke, A. Complications of lumbar administration of 5% sodium fluorescein solution for detection of cerebrospinal fluid fistula. Laryngo-rhino-otologie. 82 (12), 833-838 (2003).
- Harley, B., et al. Endoscopic transnasal repair of two cases of spontaneous cerebrospinal fluid fistula in the foramen rotundum. Journal of Clinical Neuroscience: Official Journal of the Neurosurgical Society of Australia. 59, 350-352 (2019).
- Wolf, G., Greistorfer, K., Stammberger, H. Endoscopic detection of cerebrospinal fluid fistulas with a fluorescence technique. Report of experiences with over 925 cases. Laryngo-rhino-otologie. 76 (10), 588-594 (1997).



