- 00:00Overview
- 00:53Principles Behind the Continuous Wave HHD Device
- 05:00Lower Extremity Arterial Assessment
- 06:51Determining Ankle Brachial Pulse Index (ABPI)
- 10:18Testing Venous insufficiency
- 11:53Summary
Peripheral Vascular Exam Using a Continuous Wave Doppler
English
Share
Overview
Source: Joseph Donroe, MD, Internal Medicine and Pediatrics, Yale School of Medicine, New Haven, CT
Peripheral vascular disease (PVD) is a common condition affecting older adults and includes disease of the peripheral arteries and veins. While the history and physical exam offer clues to its diagnosis, Doppler ultrasound has become a routine part of the bedside vascular examination. The video titled "The Peripheral Vascular Exam" gave a detailed review of the physical examination of the peripheral arterial and venous systems. This video specifically reviews the bedside assessment of peripheral arterial disease (PAD) and chronic venous insufficiency using a handheld continuous wave Doppler.
The handheld Doppler (HHD) is a simple instrument that utilizes continuous transmission and reception of ultrasound (also referred to as continuous wave Doppler) to detect changes in blood velocity as it courses through a vessel. The Doppler probe contains a transmitting element that emits ultrasound and a receiving element that detects ultrasound waves (Figure 1). The emitted ultrasound is reflected off of moving blood and back to the probe at a frequency directly related to the velocity of blood flow. The reflected signal is detected and transduced to an audible sound with a frequency directly related to that of the received Doppler signal (thus, faster blood flow produces a higher frequency sound).
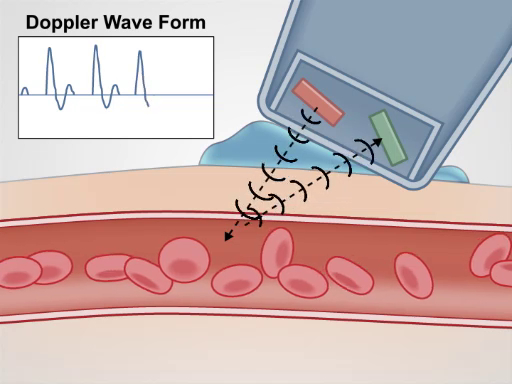
Figure 1. Generation of a Doppler signal. The handheld Doppler emits an ultrasound signal, which is then reflected back by moving blood, and finally received by the Doppler probe.
The HHD is easily used in the office or hospital setting to detect pulses, screen for PAD using the ankle brachial pressure index (ABPI), and localize venous insufficiency. This video reviews these procedures; however, it is not intended to be a comprehensive review of non-invasive vascular testing.
Procedure
1. Preparation
- Obtain a blood pressure cuff, an HHD machine, Doppler gel, and skin marker.
- Wash hands prior to examining the patient.
- Begin with the patient in a gown, lying comfortably supine on the exam table.

Figure 2. The major arteries of the upper and lower extremities.
2. Lower Extremity Arterial Assessment
- For patients with weak or absent pulses by palpation, or historical risk factors for peripheral arterial disease (PAD), use the HHD to assess blood flow. Begin by applying gel in the expected area of the artery being investigated ( Figure 2).
- Place the Doppler over the artery at a 45 degree angle to the skin, pointing cephalad. If the Doppler signal is not detected, slowly move the Doppler probe medially and laterally, as occasionally, the path of distal arteries can vary. Remember that a small percentage of people may have a congenitally absent dorsalis pedal (DP) artery.
- If a signal is encountered, note the character of the sound wave produced. While some HHD have a screen or can print out the waveform to view, the shape can also be determined by listening. A normal arterial waveform in the lower extremity is triphasic (Figure 3). The first component of the wave occurs in systole and is generated by the rapid flow of blood toward the probe, generating a high frequency wave. At the end of systole and beginning of diastole, blood flow slows and reverses direction, resulting in a second, lower frequency wave. Finally, forward returns at the end of diastole, producing the low frequency third wave. Distal to an arterial stenosis, the amplitude of the waveform becomes progressively dampened with loss of flow reversal, resulting in a monophasic waveform. Immediately over a partially stenosed segment of artery, the flow velocity is increased, producing a high frequency wave. Complete arterial occlusion without collateral flow leads to absence of flow distally and no signal generation.

Figure 3. The triphasic Doppler arterial waveform. The initial large deflection is forward blood flow during systole. The second deflection is the reversal of flow in early diastole. The third deflection is return of forward flow in late diastole.
- If frequent reassessment is necessary, mark the location where the arterial pulse is found.
- If there is suspicion for peripheral arterial disease based on the history or physical exam, calculate the ankle brachial pulse index (ABPI). Prior to performing the procedure, have the patient lie supine and relax for 10 min, with both the upper and lower extremities at the level of the heart.
- Place the appropriately-sized blood pressure (BP) cuff on the upper arm. Make sure the cuff bladder length is at least 80% and the bladder width at least 40% of the arm circumference.
- Apply gel to the antecubital fossa medial to the biceps tendon and find the brachial artery with the HHD.
- Inflate the cuff until the Doppler signal disappears.
- Slowly deflate the cuff. The first Doppler signal heard reflects the systolic pressure. Record this number and repeat the process in the other arm.
- Place the appropriately sized BP cuff on the lower extremity, just proximal to the ankle.
- Apply gel to the dorsum of the foot lateral to the extensor hallucis longus tendon and use the HHD to find the DP artery.
- Inflate the cuff until the Doppler signal disappears.
- Slowly deflate the cuff. The first Doppler signal heard reflects the systolic pressure. Record this number and repeat the process over the posterior tibialis (PT) artery.
- Repeat this on the other leg.
- Calculate the ABPI for a given leg by dividing the higher systolic pressure of the DP or PT artery in that leg with the higher of the two brachial artery systolic pressures. Table 1 shows the interpretation of the ABPI.
| ABPI of leg A = Higher pedal pressure of leg A / Higher brachial pressure (A or B) | |
| Value | Interpretation |
| >1.4 | Non-compressible, calcified arteries |
| 1.0-1.4 | Normal range |
| 0.91-0.99 | Borderline |
| 0.41-0.90 | Mild to moderate peripheral arterial disease |
| <0.4 | Severe peripheral arterial disease |
Table 1: Interpretation of the Ankle Brachial Pressure Index (ABPI).
- Assess for venous insufficiency of the lower extremity in patients with edema or varicose veins. Have the patient in the standing position with their weight shifted onto the unexamined leg.
- Apply a generous amount of gel and place the HHD over the femoral artery, just below the inguinal ligament. Slowly move the probe medially, while squeezing and releasing the ipsilateral calf muscle to generate audible flow through the venous system. Once the HHD transmits this signal clearly, it is in the vicinity of the saphenofemoral junction (SFJ).
- Move just inferior and medial to the SFJ to isolate the distal segment of the greater saphenous vein (GSV).
- Squeeze the calf muscle and listen for normal augmentation of flow.
- Release the calf muscle. Re-augmentation of flow lasting more than 1 sec is abnormal and represents retrograde flow through an incompetent valve at the SFJ.
- Move to the medial thigh, approximately 10 cm above the knee along the expected path of the GSV, and apply gel.
- Place the probe on the skin, while squeezing the calf muscle. The probe is well positioned once a clear signal is heard.
- Squeeze the calf muscle and listen for normal augmentation of flow.
- Release the calf muscle. Re-augmentation of flow lasting more than 1 sec may be heard with SFJ reflux, incompetent thigh perforator veins, or incompetent valves within the GSV proximal to the HHD probe.
- Move behind the patient and place gel in the popliteal fossa.
- Use the probe to find the popliteal artery, then move medially, while squeezing the calf muscle, to find the popliteal vein.
- Once well-positioned over the popliteal vein, squeeze the calf muscle and listen for normal augmentation of flow.
- Release the calf muscle. The venous anatomy around the popliteal fossa is complex, and re-augmentation of flow lasting more than 1 sec usually cannot be localized to one particular superficial or deep vein. Rather, it may represent reflux at the saphenopopliteal junction (SPJ), the small saphenous vein, tributaries of the GSV, or calf veins.
The use of continuous wave Doppler ultrasound has become a routine part of the bedside vascular assessment, complementing the patient’s history and physical examination.
This assessment is performed with a simple, non-invasive instrument called the handheld Doppler device or HHD. This device consists of a probe, which is placed on the patient’s skin to detect changes in the velocity of the blood flow as it courses through a vessel. In this presentation, we will review the principles behind the HHD device functioning, followed by a review of how to use this device to detect pulses, measure ankle brachial pressure index, and localize venous insufficiency.
Before discussing the steps of this exam, let’s briefly review the basic principles behind the functioning of the HHD device. This instrument works on the principle related to the frequency of sound waves, which was proposed almost one and a half century ago in 1842 by an Austrian physicist Christian Doppler. The principle was thus called the Doppler effect. So, what is the Doppler effect? The example commonly used to explain this phenomenon involves an observer and a sound-emitting object, like an ambulance, which produces sound waves at a constant frequency denoted by ft. Initially, when the ambulance approaches, the frequency of the sound perceived by the observer, or fr, is greater compared to ft. And, when it recedes, fr drops below ft. This difference between the perceived sound frequency and transmitted sound frequency at any given point in time is called the Doppler effect or the Doppler shift. Therefore, when the ambulance is approaching the observer the shift is positive and when it recedes the shift is negative.
The same principle applies to the continuous wave HHD device. In this case, the probe contains a transmitting element that continuously emits ultrasound waves at a constant frequency, which then reflect off of the blood cells and are detected by the receiving element in the probe. So here, a blood cell is analogous to the moving ambulance and the receiving element is analogous to the observer. Thus, the Doppler shift in the frequency experienced by the receiving element depends on two parameters: the velocity of the blood flow and the angle of the probe to the blood flow.
The velocity effect is evident when you think of the ambulance example. The faster the ambulance passes by, the greater is the change in sound frequency experienced. The angle to the blood flow is equally important, because if the probe is placed at a 45° angle to the blood flow, then the flow is towards the receiving element and hence there is a positive Doppler shift. If the probe were perpendicular, the flow would be neither towards nor away relative to the probe, therefore the Doppler shift would be zero. And if it were placed at an obtuse angle, then the flow would be actually away from the probe, which would yield in a negative Doppler shift.
Normally, one places the probe at a 45° angle to the direction of blood flow in a peripheral artery and this produces a Doppler waveform, which is triphasic in nature. First component of this wave occurs in systole and reflects the rapid blood flow toward the probe, which generates a high frequency wave. At the end of systole and beginning of diastole, blood flow slows and reverses direction, resulting in a second, lower frequency wave on the negative side. Finally, forward flow returns at the end of diastole, producing the low frequency third wave on the positive side before the process is repeated for the next cardiac cycle.
Since the triphasic waveform represents normal, deviation from it provides valuable diagnostic clues. For example, a partial arterial stenosis progressively dampens the amplitude of the waveform distally and there is loss of flow reversal resulting in a monophasic waveform. And a complete occlusion without collateral flow leads to no signal generation.
Some of the HHD devices are equipped with a screen or a printer that displays these waveforms. Others come with a built in processor that convert this waveform into audible sounds, and a triphasic wave on such a device sounds like this…
Now we will demonstrate how to use the HHD to assess the blood flow in leg arteries. You should perform this test if your patient’s symptoms and risk factors are consistent with peripheral arterial disease or if they have weak or absent peripheral pulses by palpation.
Before starting the exam have the patient wear a gown and ask them to lie on the exam table in supine position. Here, we will demonstrate how to use the Doppler device to evaluate the dorsal pedal artery, but the same principle is applicable for the assessment of other leg and arm arteries as well, including posterior tibial, popliteal, femoral, ulnar, radial and brachial arteries.
First try to find the dorsal pedal pulse by palpating just laterally to the tendon of extensor hallucis longus. After you find the pulse, apply ultrasound gel on the skin over the area. Next, place the probe over the gel at a 45° angle to the skin pointing cephalad.
Slowly move the probe both medially and laterally until you hear the signal. Remember that a small percentage of people may have a congenitally absent dorsalis pedal artery. Note the character of the sound wave. Recall-a normal arterial waveform in the lower extremity is triphasic. If your patient needs frequent reassessment of their pulses, mark the location where the arterial pulse is found with a skin marker.Use the same approach to assess peripheral arteries in both lower extremities and record the findings.
Now let’s discuss how to utilize the HHD device for measuring ankle brachial pressure index or ABPI. Since the HHD is more sensitive than auscultation, it allows for more precise measuring of blood pressure in distal arteries. And ABPI is nothing but the fraction of the systolic blood pressure in legs to the systolic blood pressure in arms. It is a way to assess the distal perfusion.
Prior to this test, have the patient lie supine and relax for 10 minutes with their upper and lower extremities positioned at the level of the heart. Obtain a sphygmomanometer attached to an appropriately sized blood pressure cuff and place the cuff on the patient’s upper arm. Identify the brachial pulse in the antecubital fossa by palpating medially to the biceps tendon. Apply the gel on the skin over the brachial pulse and then place the probe at a 45° angle to the skin pointing cephalad. Move the probe until you obtain the signal…
Now measure the systolic pressure in the brachial artery. Inflate the cuff until the Doppler signal disappears, and then continue to inflate for additional 20 mmHg above that point. Then deflate the cuff slowly, while watching the readings on the manometer. The first Doppler signal heard signifies the systolic pressure in the brachial artery. Record this manometer reading and repeat the procedure in the other arm.
Now use the same approach to measure the systolic pressure in dorsal pedal artery and tibialis posterior artery in each leg. Place the appropriately sized blood pressure cuff on the lower extremity, just proximal to the ankle. Apply gel to the dorsum of the foot, lateral to the extensor hallucis longus tendon and use the probe to find the dorsal pedal artery as shown earlier. Once you found the pulse, start inflating the cuff until the Doppler signal cannot be heard anymore. Deflate the cuff slowly and record the pressure at which the Doppler signal reappears. Then, measure the systolic pressure in the posterior tibial artery on the same side. Using the same approach, obtain systolic pressure measurements in the dorsal pedal and posterior tibial arteries of the other leg.
Calculate the ABPI for each leg separately by dividing the higher systolic pressure of the dorsal pedal or posterior tibial artery in that leg by the higher of the two brachial artery systolic pressures. The generally accepted normal range of ABPI is from 1 to 1.4. Values below 1 indicate the presence of peripheral artery disease, ranging in severity depending on the actual value. On the other end, if the value exceeds 1.4, it suggests presence of non-compressible, calcified arteries in that leg.
Finally, let’s learn how to use the HHD device for the assessment of leg veins by performing compression test for localizing valvular reflux.
Before starting this test, ask the patient to stand up and relax the leg to be examined with their weight shifted onto the other leg. Apply a generous amount of gel and place the probe over the femoral artery, just below the inguinal ligament. Then, move the probe medially, while squeezing and releasing the ipsilateral calf muscle to generate audible flow through venous system. Once the device transmits this signal clearly, the probe is in the vicinity of the saphenofemoral junction. Now, move the probe slightly medial and inferior to the junction to assess the great saphenous vein.Squeeze and release the calf muscle and listen for normal augmentation of flow. Re-augmentation of flow lasting more than one second is abnormal and represents retrograde flow through an incompetent valve at the saphenofemoral junction.
Repeat the same procedure for testing the great saphenous vein in the medial thigh, 10 cm above the knee and then for testing the popliteal vein located posteriorly in the popliteal fossa. The interpretation of the findings is described in the associated text manuscript.
You’ve just watched JoVE’s video on the peripheral vascular exam using a continuous wave Doppler device. This video demonstrated the principles behind the Doppler device, showed how to perform bedside assessment of peripheral vascular system using this simple, portable device and explained how to interpret the results obtained. As always, thanks for watching!
Applications and Summary
A careful history and physical exam are important for anyone suspected of peripheral vascular disease based on symptoms or risk factors. The HHD has become part of the routine bedside vascular examination and should be used to complement the physical exam, if PVD is suspected. It is not a technically difficult tool to use, and the maneuvers described in the video can be performed by general physicians. Just like for the physical exam, knowledge of the vascular anatomy is critical to the success of the HHD exam.
Vascular assessment by HHD has some important limitations. A false positive Doppler signal may occur over an artery distal to a total occlusion, if sufficient collateral flow has developed, leading to the inaccurate belief that PAD is not present. Additionally, the ABI may be falsely high in calcified vessels as they become less compressible. This is particularly relevant to diabetic patients. Venous testing by HHD is far more accurate for localizing valvular reflux than physical exam maneuvers, such as the Brodie-Trendelenburg test, cough test, and Perthes test; however, it is still less accurate than color duplex scanning. Finally, while there is some literature describing HHD testing for deep vein thrombosis, this is not considered standard of care, and thus, it is not reviewed here. If clinical suspicion for peripheral vascular disease persists despite reassuring physical exam and HHD testing, more formal vascular testing should be performed by a vascular specialist.
Transcript
The use of continuous wave Doppler ultrasound has become a routine part of the bedside vascular assessment, complementing the patient’s history and physical examination.
This assessment is performed with a simple, non-invasive instrument called the handheld Doppler device or HHD. This device consists of a probe, which is placed on the patient’s skin to detect changes in the velocity of the blood flow as it courses through a vessel. In this presentation, we will review the principles behind the HHD device functioning, followed by a review of how to use this device to detect pulses, measure ankle brachial pressure index, and localize venous insufficiency.
Before discussing the steps of this exam, let’s briefly review the basic principles behind the functioning of the HHD device. This instrument works on the principle related to the frequency of sound waves, which was proposed almost one and a half century ago in 1842 by an Austrian physicist Christian Doppler. The principle was thus called the Doppler effect. So, what is the Doppler effect? The example commonly used to explain this phenomenon involves an observer and a sound-emitting object, like an ambulance, which produces sound waves at a constant frequency denoted by ft. Initially, when the ambulance approaches, the frequency of the sound perceived by the observer, or fr, is greater compared to ft. And, when it recedes, fr drops below ft. This difference between the perceived sound frequency and transmitted sound frequency at any given point in time is called the Doppler effect or the Doppler shift. Therefore, when the ambulance is approaching the observer the shift is positive and when it recedes the shift is negative.
The same principle applies to the continuous wave HHD device. In this case, the probe contains a transmitting element that continuously emits ultrasound waves at a constant frequency, which then reflect off of the blood cells and are detected by the receiving element in the probe. So here, a blood cell is analogous to the moving ambulance and the receiving element is analogous to the observer. Thus, the Doppler shift in the frequency experienced by the receiving element depends on two parameters: the velocity of the blood flow and the angle of the probe to the blood flow.
The velocity effect is evident when you think of the ambulance example. The faster the ambulance passes by, the greater is the change in sound frequency experienced. The angle to the blood flow is equally important, because if the probe is placed at a 45° angle to the blood flow, then the flow is towards the receiving element and hence there is a positive Doppler shift. If the probe were perpendicular, the flow would be neither towards nor away relative to the probe, therefore the Doppler shift would be zero. And if it were placed at an obtuse angle, then the flow would be actually away from the probe, which would yield in a negative Doppler shift.
Normally, one places the probe at a 45° angle to the direction of blood flow in a peripheral artery and this produces a Doppler waveform, which is triphasic in nature. First component of this wave occurs in systole and reflects the rapid blood flow toward the probe, which generates a high frequency wave. At the end of systole and beginning of diastole, blood flow slows and reverses direction, resulting in a second, lower frequency wave on the negative side. Finally, forward flow returns at the end of diastole, producing the low frequency third wave on the positive side before the process is repeated for the next cardiac cycle.
Since the triphasic waveform represents normal, deviation from it provides valuable diagnostic clues. For example, a partial arterial stenosis progressively dampens the amplitude of the waveform distally and there is loss of flow reversal resulting in a monophasic waveform. And a complete occlusion without collateral flow leads to no signal generation.
Some of the HHD devices are equipped with a screen or a printer that displays these waveforms. Others come with a built in processor that convert this waveform into audible sounds, and a triphasic wave on such a device sounds like this…
Now we will demonstrate how to use the HHD to assess the blood flow in leg arteries. You should perform this test if your patient’s symptoms and risk factors are consistent with peripheral arterial disease or if they have weak or absent peripheral pulses by palpation.
Before starting the exam have the patient wear a gown and ask them to lie on the exam table in supine position. Here, we will demonstrate how to use the Doppler device to evaluate the dorsal pedal artery, but the same principle is applicable for the assessment of other leg and arm arteries as well, including posterior tibial, popliteal, femoral, ulnar, radial and brachial arteries.
First try to find the dorsal pedal pulse by palpating just laterally to the tendon of extensor hallucis longus. After you find the pulse, apply ultrasound gel on the skin over the area. Next, place the probe over the gel at a 45° angle to the skin pointing cephalad.
Slowly move the probe both medially and laterally until you hear the signal. Remember that a small percentage of people may have a congenitally absent dorsalis pedal artery. Note the character of the sound wave. Recall-a normal arterial waveform in the lower extremity is triphasic. If your patient needs frequent reassessment of their pulses, mark the location where the arterial pulse is found with a skin marker.Use the same approach to assess peripheral arteries in both lower extremities and record the findings.
Now let’s discuss how to utilize the HHD device for measuring ankle brachial pressure index or ABPI. Since the HHD is more sensitive than auscultation, it allows for more precise measuring of blood pressure in distal arteries. And ABPI is nothing but the fraction of the systolic blood pressure in legs to the systolic blood pressure in arms. It is a way to assess the distal perfusion.
Prior to this test, have the patient lie supine and relax for 10 minutes with their upper and lower extremities positioned at the level of the heart. Obtain a sphygmomanometer attached to an appropriately sized blood pressure cuff and place the cuff on the patient’s upper arm. Identify the brachial pulse in the antecubital fossa by palpating medially to the biceps tendon. Apply the gel on the skin over the brachial pulse and then place the probe at a 45° angle to the skin pointing cephalad. Move the probe until you obtain the signal…
Now measure the systolic pressure in the brachial artery. Inflate the cuff until the Doppler signal disappears, and then continue to inflate for additional 20 mmHg above that point. Then deflate the cuff slowly, while watching the readings on the manometer. The first Doppler signal heard signifies the systolic pressure in the brachial artery. Record this manometer reading and repeat the procedure in the other arm.
Now use the same approach to measure the systolic pressure in dorsal pedal artery and tibialis posterior artery in each leg. Place the appropriately sized blood pressure cuff on the lower extremity, just proximal to the ankle. Apply gel to the dorsum of the foot, lateral to the extensor hallucis longus tendon and use the probe to find the dorsal pedal artery as shown earlier. Once you found the pulse, start inflating the cuff until the Doppler signal cannot be heard anymore. Deflate the cuff slowly and record the pressure at which the Doppler signal reappears. Then, measure the systolic pressure in the posterior tibial artery on the same side. Using the same approach, obtain systolic pressure measurements in the dorsal pedal and posterior tibial arteries of the other leg.
Calculate the ABPI for each leg separately by dividing the higher systolic pressure of the dorsal pedal or posterior tibial artery in that leg by the higher of the two brachial artery systolic pressures. The generally accepted normal range of ABPI is from 1 to 1.4. Values below 1 indicate the presence of peripheral artery disease, ranging in severity depending on the actual value. On the other end, if the value exceeds 1.4, it suggests presence of non-compressible, calcified arteries in that leg.
Finally, let’s learn how to use the HHD device for the assessment of leg veins by performing compression test for localizing valvular reflux.
Before starting this test, ask the patient to stand up and relax the leg to be examined with their weight shifted onto the other leg. Apply a generous amount of gel and place the probe over the femoral artery, just below the inguinal ligament. Then, move the probe medially, while squeezing and releasing the ipsilateral calf muscle to generate audible flow through venous system. Once the device transmits this signal clearly, the probe is in the vicinity of the saphenofemoral junction. Now, move the probe slightly medial and inferior to the junction to assess the great saphenous vein.Squeeze and release the calf muscle and listen for normal augmentation of flow. Re-augmentation of flow lasting more than one second is abnormal and represents retrograde flow through an incompetent valve at the saphenofemoral junction.
Repeat the same procedure for testing the great saphenous vein in the medial thigh, 10 cm above the knee and then for testing the popliteal vein located posteriorly in the popliteal fossa. The interpretation of the findings is described in the associated text manuscript.
You’ve just watched JoVE’s video on the peripheral vascular exam using a continuous wave Doppler device. This video demonstrated the principles behind the Doppler device, showed how to perform bedside assessment of peripheral vascular system using this simple, portable device and explained how to interpret the results obtained. As always, thanks for watching!
