Three-dimensional Confocal Analysis of Microglia/macrophage Markers of Polarization in Experimental Brain Injury
Summary
A way to gain new insights into the complexity of the brain inflammatory response is presented. We describe immunofluorescence-based protocols followed by three-dimensional confocal analysis to investigate the pattern of co-expression of microglia/macrophage phenotype markers in a mouse model of focal ischemia.
Abstract
After brain stroke microglia/macrophages (M/M) undergo rapid activation with dramatic morphological and phenotypic changes that include expression of novel surface antigens and production of mediators that build up and maintain the inflammatory response. Emerging evidence indicates that M/M are highly plastic cells that can assume classic pro-inflammatory (M1) or alternative anti-inflammatory (M2) activation after acute brain injury. However a complete characterization of M/M phenotype marker expression, their colocalization and temporal evolution in the injured brain is still missing.
Immunofluorescence protocols specifically staining relevant markers of M/M activation can be performed in the ischemic brain. Here we present immunofluorescence-based protocols followed by three-dimensional confocal analysis as a powerful approach to investigate the pattern of localization and co-expression of M/M phenotype markers such as CD11b, CD68, Ym1, in mouse model of focal ischemia induced by permanent occlusion of the middle cerebral artery (pMCAO). Two-dimensional analysis of the stained area reveals that each marker is associated to a defined M/M morphology and has a given localization in the ischemic lesion. Patterns of M/M phenotype marker co-expression can be assessed by three-dimensional confocal imaging in the ischemic area. Images can be acquired over a defined volume (10 μm z-axis and a 0.23 μm step size, corresponding to a 180 x 135 x 10 μm volume) with a sequential scanning mode to minimize bleed-through effects and avoid wavelength overlapping. Images are then processed to obtain three-dimensional renderings by means of Imaris software. Solid view of three dimensional renderings allows the definition of marker expression in clusters of cells. We show that M/M have the ability to differentiate towards a multitude of phenotypes, depending on the location in the lesion site and time after injury.
Introduction
After acute brain injury, microglia are rapidly activated and undergo dramatic morphological and phenotypic changes1-3. This intrinsic response is associated to recruitment of blood-born macrophages which migrate into the injured brain parenchyma4,5. The role of microglia and macrophages which are antigenically not distinguishable (henceforth referred to as M/M) in brain injury is still debated. An increasing number of studies indicate that, similarly to what described for peripheral macrophages, microglia and brain recruited macrophages can assume different phenotypes whose extremes correspond to classic pro-inflammatory toxic (M1) or anti-inflammatory protective (M2) phenotype. The different activation states, including secretion of pro- or anti-inflammatory factors, release of neurotrophic molecules and lysosomal activity are characterized by a specific pattern of phenotypic markers, whose expression depends on the temporal evolution of the surrounding environment. The characterization of these M/M phenotypes in the injured brain is still scanty. We used a well-established murine model of pMCAo to analyze M/M expression and evolution after stroke. Immunofluorescence based protocols presented here aim at getting insight into the appearance of specific M/M phenotype markers, their localization and cellular co-expression in the ischemic area. We investigated a few molecules associated to different activation state or phenotype, namely CD11b, a surface marker expressed by leukocytes and a widely used marker of M/M activation/recruitment6-8, CD68 a marker of lysosomes6,7 and Ym1 a secretory protein expressed by alternatively activated (M2) macrophages and associated to recovery and function restoration9-10.
When two markers are expressed by the same cell, but in different subcellular compartments, colocalization alone may not be much informative. In this case, analysis of coexpression can be performed by using single plane view and by three-dimensional renderings. We here describe a protocol to obtain a thorough three-dimensional analysis of marker coexpression.
Protocol
1. Immunofluorescence
The following protocol is performed on coronal brain cryosections obtained from transcardially perfused mice (20 ml of PBS, 0.1 mol/liter, pH 7.4, followed by 50 ml of chilled paraformaldehyde 4% in PBS). After perfusion, brains are carefully removed and transferred to 30% sucrose in PBS at 4 °C overnight for cryoprotection. The brains are then rapidly frozen by immersion in isopentane at – 45 °C for 3 min before being sealed into vials and stored at -70 °C until use. Coronal brain cryosections (20 μm) are cut serially and subjected to immunofluorescence protocol 11, 6.
Bring all reagents and samples to room temperature before use. Please note that the presented working dilutions of antibodies and serum resulted from trials made in order to obtain the best performance. When different antibodies and serum are used, the protocol needs to be validated.
Note that because both anti-CD11b and anti-CD68 primary antibodies are made in rat, to avoid cross signal by anti-rat Alexa 546, we used a high dilution of anti-CD11b followed by fluorescent signal amplification with TSA kit (Cy5 Tyramide). We have set up the optimal working dilution for anti-CD11b by performing the described protocol except for step 1.17 and using at least 7 different dilutions of anti-CD11b as reported in table 1. As a result, 1:30,000 has been chosen being the only dilution achieving: 1) visible signal with Cy5 at excitation wavelength 646 nm; 2) no signal with Alexa 546 at excitation wavelength 532 nm. In this way, Alexa 546 fluorescent signal is selectively associated with CD68 expression.
The optimal dilutions for anti-CD11b and anti-CD68 antibodies may vary depending on the type of tissue and must be defined prior to start the co-labeling protocol.
- Wash brain cryosections twice with PBS.
- Incubate cryosections for 5 min in PBS containing 1% H2O2 (step required since the fluorescent amplification needs incubation with horseradish peroxidase, streptavidin-HRP, see step 1.12).
- Wash cryosections 2x with PBS.
- Incubate cryosections for 60 min in PBS containing 10% NGS and 0.3% Triton.
- Incubate cryosections at 4 °C overnight in PBS containing primary Ab Rat anti-CD11b [1:30,000], 10% NGS and 0.3% Triton.
- Wash cryosections 2x (5 min) with PBS.
- Incubate cryosections for 60 min in PBS containing biotinylated secondary anti-Rat Ab [1:200] and 1% NGS.
- Wash cryosections 2x with PBS.
- Wash cryosections with TNT (Tris-HCl, NaCl, Tween: 0.1 M TRIS-HCl, pH 7.4, 0.15 M NaCl, 0.05% Tween 20).
- Incubate cryosections for 1.5 hr in TNB (Tris-HCl-NaCl-Blocking buffer: 0.1 M TRIS-HCl, pH 7.4, 0.15 M NaCl, 0.5% Blocking reagent from appropriate kit (see table of reagents)).
- Wash cryosections 3x times with TNT.
- Incubate cryosections in TNB containing streptavidin-HRP [1:100].
- Wash cryosections 3x with TNT.
- Incubate cryosections for 8 min in Amplification Diluent containing Cyanine 5 Tyramide [1:300].
- Wash cryosections 3x with PBS.
- Incubate cryosections for 60 min in PBS containing 10% NGS and 0.1% Triton.
- Incubate cryosections at 4 °C overnight in PBS containing primary Ab Rat anti-CD68 [1:200], 3% NGS and 0.3% Triton.
- Wash cryosections 3x with PBS.
- Incubate cryosections for 60 min in PBS containing fluorconjugated secondary Ab Alexa 546 anti-Rat [1:500] and 1% NGS.
- Wash cryosections 3x with PBS.
- Incubate cryosections for 10 min in PBS containing Hoechst 1 μg/ml.
- Wash cryosections 3x with PBS.
- Mount cryosections in Prolong Gold.
2. Acquisition of Three-dimensional Images by Confocal Microscopy
The microscope used here was a IX81 microscope equipped with a confocal scan unit FV500 with 3 laser lines: Ar-Kr (488nm), He-Ne red (646nm), and He-Ne green (532nm) and a UV diode.
- Select the excitation lasers depending on the wavelengths of the fluorescent dyes to be excited (He-Ne red for Cy5, CD11b; He-Ne green for Alexa546, CD68 and the UV diode for Hoechst, nuclei).
- Select the best dichroic mirror combination for light signal collection.
- Set up image resolution at a minimum of 800 x 600 pixels.
- Identify an area of interest by using epi-fluorescence and progressively increase the magnification to the 40X objective.
- Switch to Laser Scanning Microscopy (LSM) modality.
- Run repetitive scans to adjust the photomultiplier (PMT) and the gain for each channel. Lasers may be turned on individually to facilitate the set up. Keep gain as low as possible to avoid unwanted non-specific signals.
- With repetitive scan running, move the focus control to define lower and upper extremes of the z-axis (total z-axis length = 10 μm).
- Stop repetitive scan.
- Define step size. It should be as close as possible to pixel size (0.225 μm) to obtain a standard 1:1 size ratio over the z-axis.
- Activate Kalman filter at least 2 times.
- Activate sequential scanning mode to avoid bleed-through effects.
- Go half-way along the z-axis and run a xy sequential scan. Check the set-up of PMT and gain (good signal/noise ratio). If not satisfactory, repeat step 2.6.
- Run xyz acquisition.
- Export data as multitiff file. Each multitiff file typically contains 3 color channels (blue, green and red) and 44 focal planes.
3. Three-dimensional View of Confocal Acquisitions and Three-dimensional Rendering
Upload multitiff files to Imaris software and process them as follows:
- Open software.
- Select the surpass view.
- Upload the multitiff file.
- Select the desired color for each channel.
- Remove noise from background by increasing the minimum value on the display adjustment panel. Adjust each channel individually.
- Go to the section view. Move along the z-axis looking for co-localization (yellow pixels).
- Click on a yellow area to see whether the colocalization is present along the z-axis (i.e. belongs to a solid object). Z-axis projections are visible in the right and bottom part of the figure.
- Take a snapshot.
- Go back to surpass view.
- Crop 3D to isolate a cell or a cluster of cells.
- Select one channel on the display adjustment panel.
- Select the surpass/surfaces algorithm builder. Algorithm steps:
- Select channel.
- Define threshold (use the same minimum value in the display adjustment panel).
- Define resizing.
- Define smoothing (best = 0.200).
- Define color appearance.
- End algorithm.
- Repeat step 3.12 for each channel.
- Deselect fluorescence channels on the display adjustment panel and select all the three surfaces.
- Move the volume to find the best view.
- Take a snapshot.
Representative Results
An example of the results obtained when labeling protocols and confocal acquisitions are carried out into the ischemic region is illustrated in Figures 1A and 1B. A two dimensional view of acquired images shows that at twenty-four hours after ischemia (A), the lysosomal marker CD68 (green) is expressed in hypertrophic ameboid CD11b cells (red) present in the ischemic core. In the border zone (B) CD11b positive cells display round cell bodies and ramified processes positive to CD68. Z-axis projections (right and bottom part of A and B) allow visualization of whether the marker distribution documented in the single plane view is also present along the z-axis. Where colocalization occurs, yellow pixels are generated. CD11b is the receptor for C3 fragments and exhibits a membrane distribution. CD68 labels lysosomes and is thus present mainly in the cytosol. CD11b/CD68 double positive cells usually have a small percentage of colocalized voxels and in most cases CD11b surrounds CD68 (Figure 1A). Only when phagosomes are bound to cell membrane during the phagocytic process, colocalization between CD11b and CD68 is realized (Figure 1B).
In Figure 2, the image processing that leads to the definition of marker coexpression is reported. In A, the three-dimensional view of confocal acquired images indicates the presence of CD68 positive cell (green) and Ym1 (red) positive cell, but it may not be used for the definition of colocalization. Indeed, fluorescent voxels laying parallel to the observer's view may yield a colocalized signal (yellow), that may not be related to the actual distance between markers (they are not solid objects and there may be transparency effects). To define colocalization, a single plane view with projections of the z-axis should be preferred (B). Moving along the Z-axis looking for colocalization (yellow pixels), the Z-axis projection is obtained (visible to the right and bottom part of B). Fluorescent voxels can be turn into solid objects by three-dimensional rendering (Figure 2C). The rotation of the volume allows the best view (from C' to C''''') for looking at the objects and properly assign marker expression to a specific cellular body. High magnification and solid view of three-dimensional renderings enable to define marker expression in clusters of cells (D-D''). After high magnification and 3D rendering, the two markers (CD68 and Ym1) appear to belong to different cells although in close proximity.
An example of the evaluation of the of M/M phenotype marker coexpression in the ischemic area is shown in Figure 3. Coexpression of CD11b (red), a marker of M/M activation/recruitment, CD68 (green) a marker associated with lysosomes as well as Ym1, expressed by alternative activated M/M are investigated in the ischemic area. To provide details on the functional status of M/M, we assessed their relationship with neurons (NeuN, in blue). Images of the sampled area (Figures 3A-3D) are evaluated as three-dimensional objects (Figures 3A'-3D'). CD11b/CD68 double positive cells are examined by three-dimensional rendering (Figures 3A' and 3B'). Analysis reveals that neurons (blue) are often enwrapped by CD11b positive cells in both ischemic core and border zone at 24 hr after ischemia. In most cases CD11b cells surrounding neurons are positive for CD68 at both zones, suggesting that these cells are engaged in active phagocytosis. None of the CD11b/Ym1 double positive cells (Figures 3C and 3C') appear to engage a phagocytic interaction with neurons, being CD11b/Ym1 double positive cells never in contact with NeuN positive cells.
| anti-CD11b | TSA amplification (Cy5) λ=646 nm | Alexa 546 anti-rat λ=532 nm |
| 1:800 | + | + |
| 1:1.500 | + | + |
| 1:3,000 | + | + |
| 1:5,000 | + | + |
| 1:10,000 | + | + |
| 1:30,000 | + | – |
| 1:40,000 | – | – |
Table 1. Fine tuning of working dilution for rat anti-CD11b antibody.

Figure 1. Coexpression of CD11b (red) and CD68 (green) 24 hr after pMCAO. Confocal microscopy for CD11b and CD68 shows that in the ischemic core CD11b cells are prevalently globular and some of them are positive to CD68 (A). In the border zone (B) both rounded and ramified CD11b cells are positive to CD68. Nuclei are in blue. Bars: 20 μm.

Figure 2. Coexpression of CD68 (green) and Ym1 (red) at 24 hr after pMCAO. Three-dimensional view of a confocal image acquired in the ischemic area, CD68 (green), Ym1 (red) and nuclei (blue) (A). Single plane view with z-axis projections excludes the presence of colocalized voxels (no yellow signal, B). Three-dimensional rendering turns fluorescent voxels into solid objects (C). The volume is rotated to find the best view (C'-C''''). Closer look to a cluster of cells (D). Three-dimensional rendering helps to define whether the markers are expressed by the same cell in the case of a cluster of cells (D'). CD68 and Ym1, although in close contact, are not coexpressed by the same cells, being clearly associated with different nuclei (D''). Bars: 5 μm. Click here to view larger figure.
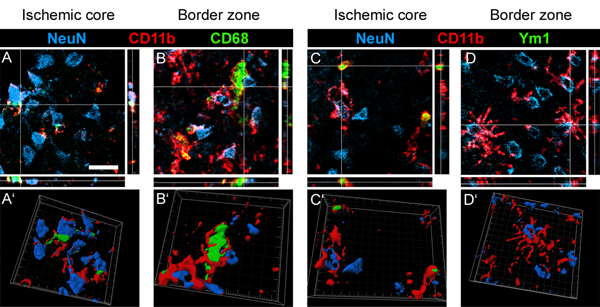
Figure 3. Coexpression of CD11b (red) and NeuN (blue) with CD68 (green) or with Ym1 at 24 hr after pMCAO. Confocal microscopy in the ischemic core (A; 3D rendering in A') and in border zone (B-B') reveals that CD11b/CD68 double positive cells envelop NeuN positive cells, possibly indicating phagocytosis of neurons. Ym1 positive cells are exclusively located into the ischemic core (C-D). Confocal analysis of CD11b/Ym1 double positive cells shows that they do not appear involved in a phagocytic interaction with neurons (NeuN positive cells, C; 3D rendering in C'). CD11b single positive cells in both ischemic core (C-C') and border zone (D-D') surround neurons. Bar: 20 μm. Click here to view larger figure.
Discussion
We present here immunofluorescence-based protocols followed by three-dimensional confocal analysis as a powerful approach to investigate localization and co-expression of M/M phenotype markers into the ischemic area (for a more detailed analysis see ref 6). This method combines specific staining of relevant marker of M/M activation with three-dimensional confocal imaging. The fine tuning of antibodies, serum and fluorconjugated working dilutions allows optimal signal to noise ratio of the investigated markers. Image processing to obtain three dimensional renderings allows definition of marker expression in cluster of cells, making acquired images indicative of the functional status of M/M. An increasing number of studies now agree that M/M are highly plastic cells that can acquire diverse phenotypes and engage different functional programs depending on surrounding signals. The inflammatory milieu evolves over time and may orchestrate the polarization of M/M, making the in vivo studies far more instructive than in vitro models, in which the complete network of recruited/activated cells cannot be reproduced.
Modifications and troubleshooting
The protocols presented here have been specifically developed on mouse brain cryosections (20 μm). Working dilutions and antibodies used may be modified according to the animal species or to the nature of tissue considered. In addition, the immunofluorescence protocol can be modified to include neuron colabeling. In this case steps 1.17 and 1.19 of the protocol may be modified as follows:
- Incubate at 4 °C overnight in PBS containing primary Ab Rat anti-CD68 [1:200], primary Ab mouse anti-NeuN [1:100], 3% NGS and 0.3% Triton.
- Incubate for 60 min in PBS containing fluorconjugated secondary Ab Alexa 546 anti-Rat [1:500], Ab Alexa 488 anti-mouse [1:500] and 1% NGS.
You may add antibodies other than anti-NeuN for detecting other antigens. In this case consider antibodies obtained in species different from rat to avoid cross reactivity with secondary antibodies. Consider also secondary Alexa antibodies with an excitation-emission spectra not-overlapping with the other dyes used.
The protocol for three-dimensional confocal acquisition may be modified (i.e. increasing the z-axis length) so as to obtain thicker image volumes (step 2.7). Keep a 1:1 pixel ratio on z-axis (step 2.9).
Critical steps within the protocol
Immunofluorescence protocols need to be validated by performing the appropriate negative controls. A negative control should be performed by omitting the primary antibody or by using a primary antibody which does not react with the species of the analyzed sample and which has the same isotype and constant region (i.e. obtained in the same immunized species) of the antibody of interest.
In double fluorescence staining where two antibodies from the same immunized species are used, the appropriate negative control must be performed by omitting only the second primary antibody used. If you are working on tissues obtained at different time points, perform the negative control at each time point, as M/M marker expression may vary over time.
Limitations of the technique
Three-dimensional confocal imaging may not provide a representative picture of the whole injured area. Even though three-dimensional analysis yields a reliable representation of M/M marker expression within specific cells, this may not be extended the whole M/M population present in the area of interest. To overcome this limit, you should provide a sufficient sampling of the brain area of interest, possibly using a motorized microscope stage to perform unbiased tissue sampling. Obviously, increasing the number of acquired frames per area would result in a more time-consuming procedure.
Significance with respect to existing methods
The expression of markers of M/M polarization has been previously analyzed by different technical approaches, including in vitro models (cell cultures exposed to polarizing agents), FACS analysis, MRI and spectroscopy, all associated with specific limitations. While providing information on the factors able to induce M/M polarization, in vitro models may not completely mirror the complex M/M in vivo response. It has indeed been well established that in the injured brain, activated M/M express mixed phenotypes and functions, as a result of the complex network of immune cell interactions12. FACS analysis provides a quantitative measure of the polarization state of the whole M/M population. However, a major limitation associated with this technique resides in the lack of localization of M/M markers in respect to the lesion. Furthermore the protocol to obtain cell suspensions from tissue specimens may stress cells and possibly alter their phenotype. MRI and spectroscopy allow to localize M/M cells within the brain areas in vivo, but have a low resolution power and cannot be applied for studying a wide range of M/M markers.
Three-dimensional confocal analysis provides information on the localization and co-expression of M/M phenotype markers into the ischemic area and should thus be associated with the techniques reported above to investigate M/M polarization states thoroughly.
Conclusion and future applications
The approach described is suitable for a wide range of applications in the field of stroke research as well as in other acute or chronic neurological diseases where a dual role of M/M in injury and recovery has been proposed. In addition the post-processing analysis described could be fruitfully exploited to analyze any coexpression or colocalization at cellular level or in those cases where signals need to be selectively localized in different spatial planes.
In the next future this technique could be significantly improved as more efficient equipment becomes available. Confocal microscopes could take advantage of the set-up of systems with higher sensitivity, multiple laser lines and software for automatic and fast tissue sampling. This will result in higher image quality, thicker acquired volumes and simultaneous acquisition of multiple signals with the aim of converting all the biological information into a digital image. Lastly, the development of new transgenic animal models with specific markers tagged with fluorescent reporters would allow analysis of co-expression in vivo by applying three-dimensional image analysis to two-photon microscopy.
This approach can represent a powerful tool to understand the complexity of the brain function with the perspective of developing future therapeutic strategies prone to drive a protective phenotype.
Disclosures
The authors have nothing to disclose.
Acknowledgements
Stefano Fumagalli is a fellow of the Monzino Foundation.
Materials
| Materials | |||
| Rat Anti-mouse CD11b | Kindly provided by Dr. A. Doni, Istituto Clinico Humanitas, Milan, Italy | ||
| Rat Anti-mouse CD68 | AbD Serotec | MCA 1957 | |
| Rabbit Anti-mouse Ym1 | Stem Cell Technologies | 1404 | |
| Hoechst 33342 | Life technologies | H21492 | |
| Mouse Anti-Neural Nuclei (NeuN) | CHEMICON | MAB377 | |
| Biotinilated Goat Anti-Rat antibody | Jackson Immuno Research | 112-065-143 | |
| TSA Cyanine 5 System | Perkin Elmer | NEL705A001KT | |
| Prolong Gold | Invitrogen | P36930 | |
| Anti-rat alexa 546 | Invitrogen | A-11081 | |
| Anti mouse Alexa 488 | Invitrogen | A-21121 | |
| Anti-rabbit Alexa 594 | Invitrogen | A-11037 | |
| Normal Goat Serum | Vectors Laboratories | S-1000 | |
| Tritin X-100 | Sigma | T8787 | |
| Phosphate Buffered Saline | Sigma | P4417-100 | |
| Equipment | |||
| Cryostat CM1850 | Leica | ||
| Olympus IX81 confocal microscope | Olympus | ||
| AnalySIS software | Olympus | ||
| Imaris software 5.0 | Bitplane | ||
| Photoshop cs2 | Adobe Systems | ||
| Software packages GraphPad Prism version 4.0 | GraphPad Software Inc. |
References
- Davalos, D., et al. ATP mediates rapid microglial response to local brain injury in vivo. Nat. Neurosci. 8, 752-758 (2005).
- Yenari, M. A., Kauppinen, T. M., Swanson, R. A. Microglial activation in stroke: therapeutic targets. Neurotherapeutics. 7, 378-391 (2010).
- Iadecola, C., Anrather, J. The immunology of stroke: from mechanisms to translation. Nat. Med. 17, 796-808 (2011).
- Jin, R., Yang, G., Li, G. Inflammatory mechanisms in ischemic stroke: role of inflammatory cells. J. Leukoc. Biol. 87, 779-789 (2010).
- Schilling, M., Besselmann, M., Muller, M., Strecker, J. K., Ringelstein, E. B., Kiefer, R. Predominant phagocytic activity of resident microglia over hematogenous macrophages following transient focal cerebral ischemia: an investigation using green fluorescent protein transgenic bone marrow chimeric mice. Exp. Neurol. 196, 290-297 (2005).
- Perego, C., Fumagalli, S., De Simoni, M. G. Temporal pattern of expression and colocalization of microglia/macrophage phenotype markers following brain ischemic injury in mice. Journal of Neuroinflammation. 8, 174-193 (2011).
- Zanier, E. R., et al. Human umbilical cord blood mesenchymal stem cells protect mice brain after trauma. Crit. CareMed. 39 (11), 2501-2510 (2011).
- Capone, C., et al. Neurosphere derived cells exert a neuroprotective action by changing the ischemic microenvironment. PLoS ONE. 2, e373 (2007).
- Bhatia, S., et al. Rapid host defense against Aspergillus fumigatus involves alveolar macrophages with a predominance ofalternatively activated phenotype. PLoS One. 6, e15943 (2011).
- Raes, G., Noel, W., Beschin, A., Brys, L., de Baetselier, P., Hassanzadeh, G. H. FIZZ1 and Ym as tools to discriminate between differentially activated macrophages. Dev. Immunol. 9, 151-159 (2002).
- Gesuete, R., et al. Recombinant C1 inhibitor in brain ischemic injury. Ann. Neurol. 66, 332-342 (2009).
- Sica, A., Mantovani, A. Macrophages plasticity and polarization: in vivo veritas. J. Clin. Invest. 122 (3), 787-795 (2012).

